How serious is it?
An arteriovenous malformation involves an abnormality of the smallest part of your circulatory system, the capillaries. For most people, it isn’t something that you have to think about, let alone worry about. If you do have one, why should you be concerned? What can be done to fix it? Can it be prevented?
 Definition
Definition
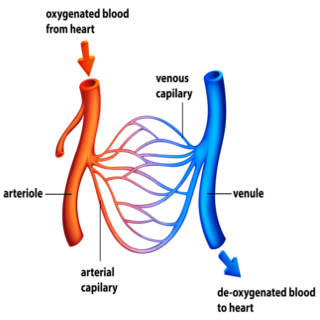
An arteriovenous malformation (AVM) involves an abnormality of your blood vessels. In order to understand how this is a problem, we need to look at the normal flow of blood throughout your body. Deoxygenated blood from your body gets pumped from the right side of your heart to your lungs so it can release carbon dioxide and pick up oxygen. Once it does this, it travels back to your heart and then gets pumped to the arteries of your body from the left side of your heart. Your arteries gradually get smaller and branch off the further they get from the heart. These smaller arteries are called arterioles. From there, they continue to decrease in size and branch off even further until the oxygenated, nutrient-rich blood reaches the arterial side of the capillaries. In the capillaries, is where the exchange of oxygen, carbon dioxide, nutrients and wastes between your blood cells and all the other cells in your body takes place. After this happens, the deoxygenated, waste-filled blood is in the venous side of the capillaries. It starts the journey back to your heart via the venules. The venules gradually get bigger and join together to form veins. The veins continue to get larger until they reach your heart. Then, the process starts all over again.
In AVM, there is an abnormal tangle in the capillaries that can form in any part of your body. Most often, it happens in your brain or spine. This tangle disrupts the process of exchange that normally occurs impacting the surrounding tissue. The tangle also can weaken the walls of the affected arteries and veins, which can lead to them rupturing. The reason why an AVM forms is unknown. If you have a family history of AVM, you have a greater chance of having it, but most types aren’t inherited.
Typically, there are no symptoms. Symptoms are usually related to the blood vessel rupturing resulting in internal bleeding. If the bleeding is significant, the symptoms can come on suddenly and can include external bleeding not the result of any injury, progressive loss of neurological function, headaches, nausea/vomiting, seizures and/or loss of consciousness. If it’s a small amount bleeding, the symptoms tend to appear gradually, but they can come on suddenly. These symptoms are weak muscles, paralysis in one part of the body, loss of coordination, problems walking, problems performing tasks that require planning, weakness in the lower extremities, back pain, dizziness, vision problems, problems with speaking or understanding what is being said to them, unusual sensations (numbness, tingling or sudden pain), memory loss/dementia, hallucinations and confusion. Sometimes, children and teenagers can have trouble learning or have behavioral problems.
Treatment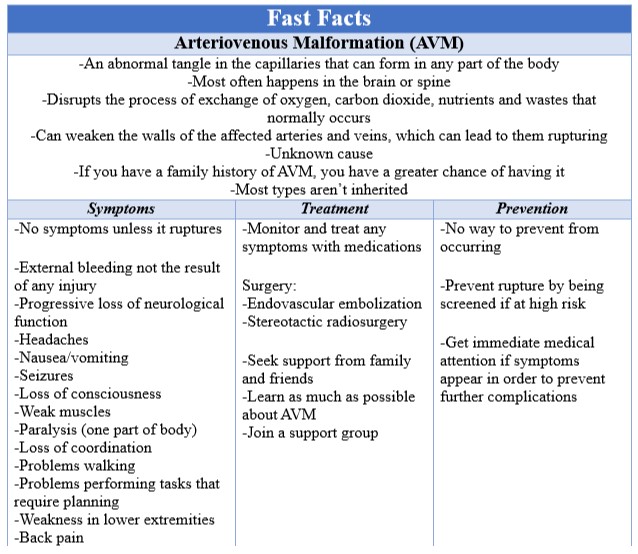
Unless you have any of the symptoms, most AVMs are found by accident when doing an imaging study, like a CT (computed tomography) scan or MRI (magnetic resonance imaging), for another reason. If you are having symptoms, your doctor can order either of these studies or a cerebral angiography, MRA (magnetic resonance angiography) or transcranial doppler ultrasound. The purpose of any of these tests is have a better visualization of your blood vessels. Once you know that you have an AVM, your doctor will help you decide what type of treatment is best for you depending on if it has bled, small enough to treat and is in a location that can be reached. Sometimes, your doctor may recommend keeping an eye on your AVM to see if it changes by doing imaging at certain time intervals (usually every few months or on a schedule set by your doctor depending on your risk level). If you in the monitoring mode, but are having seizures, headaches, back pain or other symptoms, there are medications that your doctor can prescribe to help alleviate these. If your AVM is at high risk for rupture, your doctor will probably recommend surgery. Typically, this is done if the AVM is small and in a location that surgeons can remove it with causing minimal damage to the surrounding tissue. There are two main types: endovascular embolization and stereotactic radiosurgery. In endovascular embolization, a catheter is passed through the arteries usually in your groin or neck until it reaches the area of the AVM. Once it reaches its destination, a substance is injected to form an artificial blood clot in the middle of the AVM, which temporarily reduce the blood flow to the area, but improves the blood flow around the AVM. Stereotactic radiosurgery is when an intense, highly-focused beam of radiation is used to damage the blood vessels, which stops the supply of blood to the AVM. In addition to getting treatment, it can be helpful to talk with family and friends, learn as much as you can about your AVM and join a support group to talk to others who have gone through a similar experience.
Prevention
Since the cause of AVM is unknown, there isn’t a way to prevent it from occurring. The most important to prevent is a rupture because this can be fatal. If you have a family history of AVM, talk to your doctor about getting screened. If you have any symptoms, be sure to seek medical attention immediately.
Being diagnosed with an arteriovenous malformation can be scary. The good news that there are treatments that are very successful! If you have any questions or concerns about AVM, please speak with your doctor. If you would like more information, please visit The Aneurysm and AVM Foundation page at https://www.taafonline.org/