What is wrong with your heart?
You’ve been feeling short of breath and noticed your ankles and feet have been swelling, so you go to your doctor. She tells you that you have Congestive Heart Failure and orders a bunch of tests. You’ve heard of this, but what does this mean for your health and life going forward?
 Definition
Definition
Congestive Heart Failure (CHF) occurs when your heart muscle doesn’t pump blood as well as it should. Your heart is unable to function properly because it is too weak or stiff to fill and pump efficiently. This is usually caused by narrowing of the heart arteries, known as coronary artery disease (CAD), or long term high blood pressure (hypertension). This inability to move blood out of the heart and to the rest of the body causes the blood backing up into the liver, abdomen, lower extremities and lungs. Symptoms depend on where the fluid back up is occurring and are numerous: shortness of breath (usually with exertion or while lying flat), fatigue/weakness, swelling in legs/ankles/feet, rapid/irregular heartbeat, persistent coughing/wheezing, white/pink-tinged phlegm, increased need to urinate, swelling of abdomen, sudden weight gain from fluid retention, lack of appetite/nausea, difficulty concentrating/decreased alertness and chest pain. You should see a doctor if you have any of these and they are getting worse.
Besides CAD and hypertension, there are several other risk factors that can cause CHF. If you have diabetes, previous heart attack, sleep apnea, congenital heart disease, valvular heart disease, obesity, irregular heart rhythm, use certain medications and use alcohol/tobacco, then you are at an increased risk of developing CHF. Complications associated with CHF are severe and can be kidney damage/failure (from reduction of blood flow), heart valve problems, arrhythmias and/or liver damage (from buildup of fluid putting too much pressure on liver). In order to determine the severity of CHF, it is classified on a scale of I (no impairment) to IV (severe impairment) that demonstrates how much it impacts your daily life. Please see Fast Facts for quick information about CHF symptoms and treatment.
Treatment
CHF is diagnosed by blood work (NT-proBNP), chest x-ray, ECG, Echocardiogram, stress test, CT/MRI, coronary angiogram or myocardial biopsy. Once confirmed, your doctor will initially try a plan that will manage symptoms with medications. Some medications (ACE inhibitors, 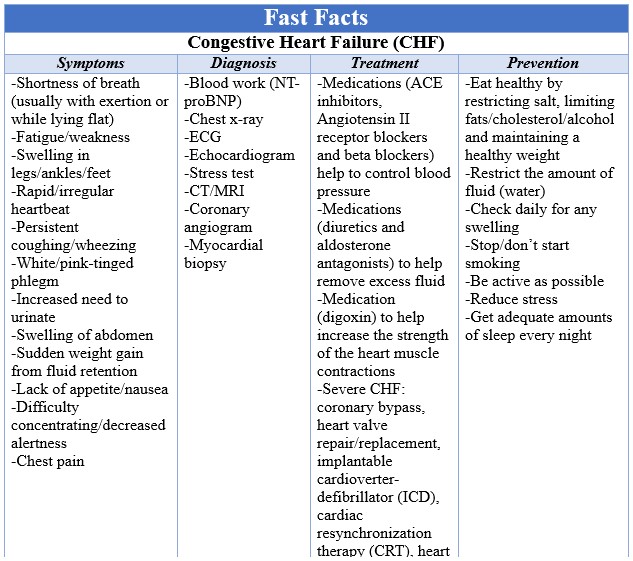 Angiotensin II receptor blockers and beta blockers) help to control blood pressure, other medications (diuretics and aldosterone antagonists) help remove excess fluid and still others (digoxin) help increase the strength of the heart muscle contractions. Often your doctor will prescribe a few of these in order for them to work together to control your CHF. If your CHF is severe, you might need coronary bypass, heart valve repair/replacement, implantable cardioverter-defibrillator (ICD), cardiac resynchronization therapy (CRT), heart pump and/or heart transplant. At home treatment is the same as prevention and will be looked at in depth in the next section. Please note that at home treatment should be used in conjunction with medicines prescribed by your doctor and should be discussed with your doctor prior to starting.
Angiotensin II receptor blockers and beta blockers) help to control blood pressure, other medications (diuretics and aldosterone antagonists) help remove excess fluid and still others (digoxin) help increase the strength of the heart muscle contractions. Often your doctor will prescribe a few of these in order for them to work together to control your CHF. If your CHF is severe, you might need coronary bypass, heart valve repair/replacement, implantable cardioverter-defibrillator (ICD), cardiac resynchronization therapy (CRT), heart pump and/or heart transplant. At home treatment is the same as prevention and will be looked at in depth in the next section. Please note that at home treatment should be used in conjunction with medicines prescribed by your doctor and should be discussed with your doctor prior to starting.
Prevention
CHF is a disease that becomes more common the older you get because it takes a long time for the damage to the heart muscle to get to the point where it starts to affect the heart’s ability to function properly. In order to prevent (and help treat the symptoms) of CHF, you should eat healthy by restricting salt, limiting fats/cholesterol/alcohol and maintaining a healthy weight. If you have CHF, you might also need to restrict the amount of fluid (water) that you take in and check daily for any swelling throughout your body. You should also stop or don’t ever start smoking. Try to be as active as possible, find ways to reduce stress and make sure you get an adequate amount of sleep every night. By doing all of these things, you will decrease your chance of having CHF and/or help maintain better control over your CHF. Always consult with your doctor prior to initiating any changes in your health plan.
You can lead a full life with CHF, but it takes an understanding of your health and the important role you can play in helping making that a reality. For further information about CHF, please visit the American Heart Association at https://www.heart.org/en/health-topics/heart-failure?