Why you should be concerned?
Everyone has heard of the word diabetes, but most people don’t realize the impact that it has on a person who lives with it daily. There are a few different types of diabetes mellitus, they are Type 1, Type 2, and Gestational. They are caused by insulin deficiency or resistance in the body. There is also disease called diabetes insipidus, which is related to the body’s inability to regulate fluid volume and composition within the body. The two diseases often present with similar symptoms, but are not the same. Let’s take a look at diabetes mellitus, which is more common and has a wider impact.
.jpg) Definition
Definition
Type 1 and Type 2 are caused by two factors, inheriting a predisposition to the disease and then something triggers it to start. In the case of Type 1, you inherit the risk factors from both parents (usually they are not diabetic). At some point, most often as a child, an environmental trigger causing the bo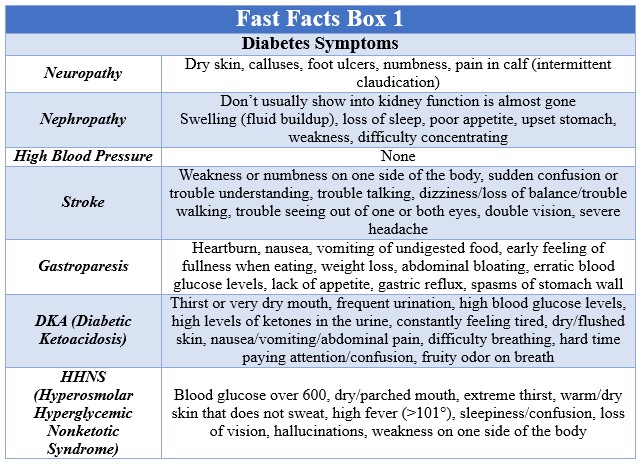 dy to become deficient at producing enough insulin. Insulin helps get the glucose (a simple sugar that is used for energy) from the food (comprised of complex sugars and starches) you eat from your bloodstream into your cells. Type 1 used to be known as juvenile diabetes because it was diagnosed most often in children versus Type 2 was more commonly identified in adults. Unfortunately in the past several years, there has been a rise in the number of children who are diagnosed with Type 2. The reason for this is that Type 2 is strongly associated with obesity, which is directly related to poor eating habits and lack of physical activity. Children learn eating and exercise habits in their family setting, so when a genetic predisposition is compounded with lifestyle choices that aren’t the healthiest, it is found that more people are having symptoms of diabetes earlier in life. Type 2 is caused by the body not using insulin properly (insulin resistance). Your pancreas, which is where insulin is produced, will make extra insulin to combat all of the extra complex sugars and starches to help break them down to glucose for a while, but eventually it can’t make enough insulin to regulate your blood glucose to normal levels.
dy to become deficient at producing enough insulin. Insulin helps get the glucose (a simple sugar that is used for energy) from the food (comprised of complex sugars and starches) you eat from your bloodstream into your cells. Type 1 used to be known as juvenile diabetes because it was diagnosed most often in children versus Type 2 was more commonly identified in adults. Unfortunately in the past several years, there has been a rise in the number of children who are diagnosed with Type 2. The reason for this is that Type 2 is strongly associated with obesity, which is directly related to poor eating habits and lack of physical activity. Children learn eating and exercise habits in their family setting, so when a genetic predisposition is compounded with lifestyle choices that aren’t the healthiest, it is found that more people are having symptoms of diabetes earlier in life. Type 2 is caused by the body not using insulin properly (insulin resistance). Your pancreas, which is where insulin is produced, will make extra insulin to combat all of the extra complex sugars and starches to help break them down to glucose for a while, but eventually it can’t make enough insulin to regulate your blood glucose to normal levels.
Gestational diabetes is most likely to present around the 24th week of pregnancy. The actual cause is unclear, but thought to be related to the hormones from the placenta that help the baby develop and grow may also block the action of the mother’s insulin in her body. This doesn’t allow the glucose to leave the bloodstream to go into the cells to provide the energy that they need (very similar to Type 2). Most often, women who have gestational diabetes do not have any problems related to diabetes prior to or will necessarily develop diabetes after giving birth (although it does increase the risk). The hazards to both the mother and baby with gestational diabetes need to be addressed, so it is important to see a doctor and receive treatment.
Symptoms and Diagnosis
Sometimes, the symptoms of diabetes are mild and go unnoticed, but the most common are urinating often, feeling very thirsty, feeling very hungry (even though you are eating), extreme fatigue, blurry vision, cuts/bruises that are slow to heal, weight loss (even though you are eating more – Type 1) and tingling/pain/numbness in the hands/feet (Type 2). Gestational diabetes often does not cause any symptoms and that is why all women who are at-risk should be tested when appropriate during pregnancy. The key with any type is early detection and treatment in order to prevent developing complications. These complications can be life threatening and include neuropathy (numbness in the feet), nephropathy (kidney disease), high blood pressure, stroke, gastroparesis (delayed stomach emptying), DKA (Diabetic Ketoacidosis – blood sugar so high it causes a coma or death), and HHNS (Hyperosmolar Hyperglycemic Nonketotic Syndrome – elevated blood sugar caused by illness or infection). All of these are important to recognize quickly in order to receive treatment as soon as possible, so please look at Fast Facts box 1 for a list of symptoms for each one of these complications.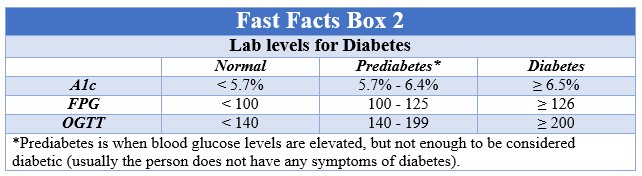
How is diabetes diagnosed before you end up with severe problems? Unfortunately, sometimes it isn’t, but the best way to avoid a problem is routine doctor’s visits, especially if you have a concern. Your doctor can order blood work which will give a clearer picture into your body’s ability to produce or use insulin. Initially, a finger stick to check your blood glucose level will be completed. If this comes back elevated, the doctor will order further testing. There are three types of blood tests (for ranges see Fast Facts box 2). A1c (or HbA1c, is the part of the hemoglobin molecule, main protein of a red blood cell, that glucose is attached to) measures your average blood glucose for the past 2 to 3 months (using one sample of blood). This does not require any fasting or you to drink any special fluids. FPG (Fasting Plasma Glucose) looks at your fasting blood glucose levels. This requires you to not have anything to eat/drink (except water) for at least 8 hours before, so usually this is done before breakfast. OGTT (Oral Glucose Tolerance Test) checks your blood glucose levels before and two hours after you drink a special sweet drink. This gives information as to how your body processes glucose.
Prevention & Living with Diabetes
Prevention is the key and maintaining an appropriate weight, eating healthy, and being physically active are the three most important things you can do. Not smoking, keeping cholesterol and blood pressure in balance, and being aware of your risk for diabetes (genetic) are also significant. Making a few small changes can make a huge difference and have a large impact on your health. All of these steps are just as essential if you already are currently living with diabetes. Always talk to your doctor prior to making any substantial changes to your diet or exercise plan. For more information about diabetes, please visit the American Diabetes Association at www.diabetes.org