What purpose does it serve?
When you are out running errands, you have probably seen signage for dialysis centers. Unless you know someone who receives dialysis, you probably aren’t aware of what goes on in these centers. What is dialysis? Why do some people need it? How do the centers help these people?
 Definition
Definition
Dialysis is used to treat kidney failure (uremia). The job of your kidneys is to filter waste products from your bloodstream. If your kidneys are unable to do this, the waste products will build up and you can die. Dialysis is the process to filter these wastes, salts and fluids from your body. By doing this, your body is able to better control your blood pressure and sustain the proper balance of fluid and minerals that your body needs. Typically, your doctor will determine when you need to start dialysis based off of your overall health, current kidney function, any symptoms you are having (ex. nausea, vomiting, swelling and fatigue), your current/desired quality of life and your personal preferences. Several elements can increase your risk of developing kidney failure and the need to start dialysis, such as diabetes, high blood pressure, kidney inflammation, blood vessel inflammation and kidney cysts. These conditions usually progress over a period of time, so the damage to your kidneys is not always evident immediately. Occasionally, your kidneys can suddenly shut down rapidly causing you to need emergent dialysis as a result. Some of the conditions that can cause a sudden kidney injury are severe illnesses, complicated surgeries, heart attacks and certain medications. The two types of dialysis are hemodialysis and peritoneal dialysis.
Hemodialysis
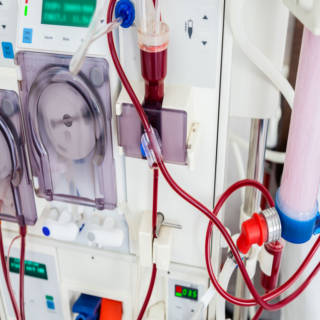
During hemodialysis, you are connected to a machine called a dialyzer and this filters your blood from your body through the machine, which cleans it, and then it is transfused back into your body. There are three types of access that allow the machine to be connected to your body. The first is a central venous catheter with two ports, which is where a plastic tube is inserted in a large vein in your neck or groin to provide access to bloodstream. This type is temporary and allows for immediate access under emergent conditions. These types are at high risk for infection, so they are mainly used in hospitals or until one of the other two options is ready to use. The second option is an arteriovenous (AV) fistula and it is when a surgeon connects an artery and a vein inside your arm (typically in your non-dominate arm). The third type is an AV graft, which is when a flexible synthetic tube is used to connect one of your arteries to one of your veins. This type is used if your blood vessels are too small to make an AV fistula. The process of hemodialysis includes inserting two needles (one in the artery side and one in the vein side) of your fistula or graft. The needles are connected to tubes that go to the dialyzer. The one side removes small amounts blood from your body at a time sending it to the machine to be cleaned and the other side receives your clean blood from the machine and infuses it back into your body. In order for the process to be completely safely, it is done slowly and your blood pressure and heart rate are monitored throughout since they can fluctuate. Each person is different in how their treatment is set up. Some people do longer sessions (three to five hours) three times a week and others do shorter sessions (two to three hours) six or seven times a week. Your doctor will decide which is better for you. Hemodialysis is a major task to undertake that requires following a strict treatment schedule, being sure to take medications regularly and changing your diet based off of your doctor’s recommendations. Dialysis centers allow people to receive the treatment they need without having to be in the hospital. Since there are centers located across the United States and in some other countries, you can travel and still get your hemodialysis. The key is to plan ahead by checking a center’s availability and making the appropriate preparations. With the advances in technology, in-home hemodialysis is becoming more popular. Regardless of where you receive hemodialysis, your doctor will monitor your weight, blood pressure, heart rate and certain blood tests (ex. urea reduction ratio, total urea clearance and blood chemistry levels) to adjust the intensity and frequency as needed.
Peritoneal Dialysis
Peritoneal dialysis is like hemodialysis in that it removes wastes from your body, but how it does it is different. It involves having a plastic tube surgically placed into your abdomen, typically near your bellybutton. After the area has healed, you will use to the tube to inject the cleaning solution (dialysate) into your abdomen. The solution stays in there for a period time (dwell time), usually four to six hours, during which it filters wastes from your body through the tiny blood vessels lining your abdominal cavity. After the dwell time has elapsed, you remove the fluid via the tube and discard it in a sterile collection bag. There are two types of schedules that are followed. Continuous ambulatory peritoneal dialysis is when you fill your abdomen with fluid and let gravity do most of the work. This type often needs to be done three to five times during a day with one longer dwell time while you’re sleeping. Continuous cycling peritoneal dialysis is when your abdomen is filled with the dialysate in the morning, the dwell time lasts all day and at night, while you are sleeping, you are connected to a machine that performs multiple exchanges. In either type, you can do your normal activities during the dwell times. Peritoneal dialysis is not an option for everyone with kidney failure. It is beneficial if your body can’t handle the rapid changes in fluid balance that affect your heart rate and blood pressure which often occurs with hemodialysis, you want to reduce the impact of dialysis on your daily activities and you have some residual kidney function. It isn’t the good choice if you have an abdominal hernia or scarring from previous abdominal surgeries, limited ability to care for yourself, diverticulitis/inflammatory bowel disease, protein malnutrition or a critical illness. Unfortunately, many people who start with peritoneal dialysis have further decline in kidney function and require hemodialysis or a kidney transplant at some point.
Dialysis is a life-altering necessity for people who have poor kidney function. Thankfully, it has become much more manageable! If you have any questions or concerns, please speak with your doctor. If you would like more information, please visit the National Kidney Foundation’s Dialysis page at https://www.kidney.org/atoz/content/dialysisinfo