Why is your skin crusty?
Thanks to TV, you’ve likely heard the word psoriasis before. However, like many people, you might not know what it is. It’s a condition that affects your skin and comes in many different forms. What does it look like? What causes it to happen? How is it treated?
 Definition
Definition
Psoriasis is a condition that occurs when the life cycle of the skin cells speeds up resulting in them rapidly building up on the surface. The cause is unknown, but thought to be related to a problem with the person’s immune system. Your immune system has many different white blood cells, each with a particular purpose. One type, T cells, normally move throughout your body protecting you from foreign objects, like viruses or bacteria. For those with psoriasis, T cells attack healthy skin by mistake, which activates an increase in healthy skin cell production, neutrophils (another type of white blood cell) and more T cells. The additional T cells continue to attack the healthy skin cells and the neutrophils cause inflammation of the area. This creates an ongoing cycle of healthy skin cells being attacked and new skin cells being formed, which results in the new skin cells moving to the outermost layer of skin too soon (in days rather than weeks). As the new skin cells get pushed outward, they form thick, silvery scales on the skin surface (called plaques). The patches can occur anywhere on your body and be small or large in size. Other symptoms include redness to the area, dry/cracked skin that bleeds, itching/burning/soreness to the area, thickened/pitted/ridged nails and swollen/stiff joints. There are several types of psoriasis. The most common is plaque psoriasis and has the classic dry, raised, red skin lesions that are covered with silvery scales, which can be itchy or painful. Nail psoriasis is when your finger and toe nails having pitting, discoloration and abnormal growth. They can loosen and separate from the nail bed and, in some case, crumble. Guttate psoriasis is activated by a bacterial infection and causes small, water-drop-shaped, scaling lesions (not at thick as plaque psoriasis) on the body. This form is more common in children. Inverse psoriasis causes smooth patches of inflamed skin in your armpits, groin, under your breasts and around your genitals. This is aggravated by friction and sweating and thought to be triggered by fungal infections. Pustular psoriasis develops quickly. At first, your skin will appear red and feel tender. Within just a few hours, you develop pus-filled blisters. The affected areas can be widespread or small. This type can also cause fever, chills, severe itching and diarrhea. The least common type is erythrodermic psoriasis, which is when your entire body is covered with a red, peeling rash that can itch or burn intensely. Sometimes, psoriasis can impact other parts of your body besides your skin. Psoriatic arthritis causes your joints to become swollen, stiff and painful similar to arthritis. It can affect any joint and range from mild to severe.
Often psoriasis will go through cycles where it flares up for a few weeks/months and then subsides for a period of time (some individuals experience complete remission). It’s thought that genetics and environmental factors contribute to the development of psoriasis. Certain things are known to trigger flare ups. Some of these potential triggers are infections, stress, injury to the skin, smoking, heavy alcohol consumption, vitamin D deficiency and certain medications. While anyone can develop psoriasis, some factors increase your risk, such as family history of psoriasis, being overweight, having a chronic immune system problem (ex. HIV) or having recurring infections. People with psoriasis are more likely to develop certain complications, like type 2 diabetes, high blood pressure, cardiovascular problems, eye conditions (ex. conjunctivitis), Parkinson’s disease, kidney disease and other autoimmune disorders (ex. celiac disease, Crohn’s disease and sclerosis).
Treatment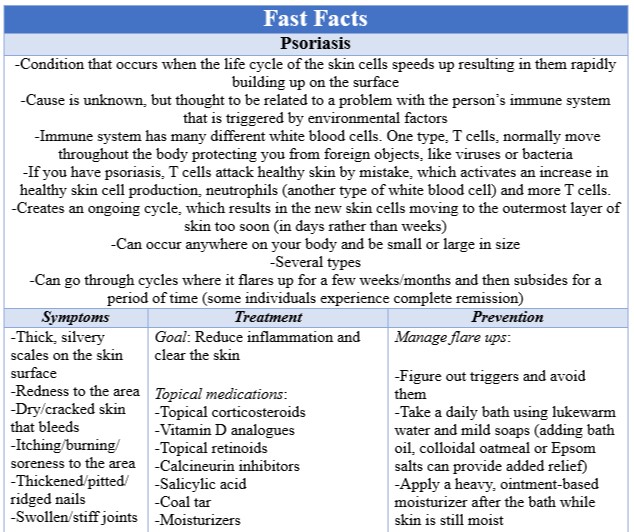
The goal of treating psoriasis is to reduce inflammation and clear the skin with the fewest amount of side effects, which means starting with the mildest treatment possible. There are three main treatment types: topical medications, light therapy and systemic medications. The initial treatment is to use creams or ointments. The most frequently prescribed are topical corticosteroids because this helps to reduce inflammation and itching. These are used mainly during flare ups. Some topical medications are designed to slow skin growth, such as vitamin D analogues or anthralin (this also removes scales and makes skin smoother—only downside is it stains anything it comes into contact with). Topical retinoids are vitamin A derivatives used to decrease inflammation. These medications make your skin more sensitive to sunlight though. Another topical medication, calcineurin inhibitors, help to reduce inflammation and plaque buildup, but aren’t recommended for long-term use since they can increase your risk for skin cancer and lymphoma. Salicylic acid encourages the sloughing of dead skin cells and reduces scaling. It’s available in prescription and non-prescription strengths. It’s often used as a medicated shampoo and scalp solutions for scalp psoriasis. Coal tar is also used for over-the-counter shampoos, creams and oils to help reduce scaling, itching and inflammation. There are some drawbacks, it’s messy causing clothing and bedding to become stained and has a strong odor. Also, women who are pregnant or breastfeeding shouldn’t use it. Some individuals find that moisturizers, especially those that are ointment-based, can help reduce itching, scaling and dryness.
If your psoriasis is mild to moderate, often topical medications are all that is need to clear it up. However, if its severe, your doctor might recommend combing these with light therapy or systemic medications. Light therapy uses natural or artificial ultraviolet light to slow skin cell growth, which reduces scaling and inflammation. Brief, daily exposure to small amounts of ultraviolet light from the sun can improve symptoms, but too much exposure can actually make symptoms worse. Broadband ultraviolet B (UVB) light can be used to treat psoriasis, especially if it’s resistant to topical treatments. Narrow band UVB therapy is a newer therapy that is thought to be more effective than broadband UVB. It’s usually only done 2-3 times a week at first. Once your skin condition improves, then you only need to go once a week. Goeckerman therapy involves putting coal tar on prior to UVB treatment because it’s thought to make the skin more receptive to the ultraviolet light. Psoralen plus ultraviolet A (PUVA) involves taking a light-sensitizing medication before being exposed to UVA. The medication makes your skin more responsive and UVA penetrates deeper into your skin. This is typically only used for more severe cases. If your psoriasis is resistant to other treatments, your doctor will recommend systemic medications, such as pills or injections. Often these medications can have major side effects. Retinoids are related to vitamin A, but can cause lip inflammation and hair loss. One in particular, acitretin, can cause such severe birth defects that women must avoid getting pregnant for at least 3 years after taking the medication. Methotrexate helps by decreasing the production of skin cells and suppressing inflammation. Cyclosporine is similar to methotrexate, but can only be taken for short periods of time due to the fact it increases your risk of infections, cancer, kidney problems and high blood pressure. Drugs that alter your immune system (or biologics) are also used for people whose psoriasis hasn’t respond to other therapies. Most of these medications are given via injection and have a significant impact on your immune system placing you at greater risk for developing life-threatening infections.
Prevention
While there isn’t a way to prevent psoriasis from occurring, there are things you can do to help manage flare ups. The first is to figure out if anything triggers a flare up and avoid it as much as possible. It’s also a good idea to take a bath daily using lukewarm water and mild soaps to remove scales and calm inflammation. Sometimes, adding bath oil, colloidal oatmeal or Epsom salts can provide added relief. After bathing, while your skin is still moist, it’s key to apply a heavy, ointment-based moisturizer. If you live in an area that experiences cold, dry weather, you’ll need to apply moisturizer several times a day. It can also be helpful to expose the areas affected by psoriasis to sunlight for brief periods. Just make sure to clear this with your doctor first and apply sunscreen to the rest of your skin. Avoid drinking alcohol and, if you do drink, don’t drink a lot. Remember, if you’re feeling self-conscious about your psoriasis, you can always cover it up with cosmetic products. It’s important to test the products on your skin first because they can cause irritation and to not use them on any open sores.
Psoriasis can be a struggle to live with each day, but by doing everything that you can to minimize flare ups, you’ll be able to have to deal with it less frequently. If you have any questions or concerns about psoriasis, please talk with your doctor. If you would like more information, please visit the National Psoriasis Foundation’s About Psoriasis page at https://www.psoriasis.org/about-psoriasis