Why is your snoring a problem?
When you hear the term sleep apnea, you probably think of someone who snores loudly at night. Sure, this is annoying, especially for family members, but it can be a serious medical problem. How do you know if you have sleep apnea? What can you do to treat or prevent it?
 Definition
Definition
Sleep apnea is when you repeatedly stop and start breathing while you’re sleeping. There are three main types classified by cause. Obstructive is the most common type. It occurs when the muscles in the back of your throat relax, causing your soft palate, uvula, tonsils, tongue, and side walls of the throat to come closer together, resulting in a narrowed opening for air to pass through when you breathe. For some people, the space actually closes completely. Central sleep apnea is less common and is when your brain doesn’t send signals to your breathing muscles, meaning you don’t breathe for short periods. Complex is a combination of the two.
The issue is the oxygen level in your blood dips from the restriction or lack of air flow. Your brain senses this and briefly awakens you so you can reopen your airway. Usually, you’re not aware of this and don’t remember being woken up. If someone is nearby while you’re sleeping, they might say you snort, gasp, or choke throughout the night. This pattern repeats all night, sometimes more than 30 times an hour. Your body can’t get the deep, restful sleep that it needs.
Regardless of the cause, the symptoms are the same. Loud snoring is the most common indication but isn’t always present. If you gasp for air while sleeping, wake up with a dry mouth, have a headache in the morning, experience insomnia, have excessive daytime sleepiness, difficulty paying attention, fatigue, or irritability, you might have sleep apnea. If family members tell you that you stop breathing at night, this is also a sign.
Anyone, even children, can have sleep apnea. The risk factors for developing it are different for each type. For obstructive, if you’re overweight, have a thicker neck, narrowed airway opening, are male, are elderly, or have a family history of sleep apnea, you’re at higher risk. Also, you are at increased risk if you smoke, use alcohol/sedatives/tranquilizers or have chronic nasal congestion. For central, if you’re male, elderly, have a heart condition, use narcotic pain medication or have a history of stroke, your risk level is elevated. For complex, it is usually a combination of obstructive and central factors.
Complications of sleep apnea are usually daytime drowsiness, fatigue, irritability, quick-tempered, moody, and depression. A worrisome complication is the chances of falling asleep at work, driving a car, or at any point during the day are significantly higher. Also, sleep apnea has a considerable impact on other areas of your health.
The drops in oxygen levels cause increases in your blood pressure and increase your chances of having a heart attack, stroke, or abnormal heart rhythms, and sometimes these are fatal. Since sleep apnea doesn’t allow you to get good, restful sleep, it doesn’t allow your body to perform certain functions that it usually does while you’re sleeping. One of the key things your body does while you’re sleeping is to regulate your glucose and insulin levels, so when it’s unable to do this because of sleep apnea, you are more likely to develop insulin resistance and type 2 diabetes. These are just a few examples of the complications that can arise; there are many others.
Treatment
To treat sleep apnea, the doctor needs to determine which type you have, which is determined using symptoms, sleep history, and diagnostic testing done at home or a sleep center. Your doctor will probably recommend lifestyle changes for milder cases, like losing weight, quitting smoking, and controlling your allergies. If these don’t work or you have moderate to severe sleep apnea, several devices can be used or procedures that can be done.
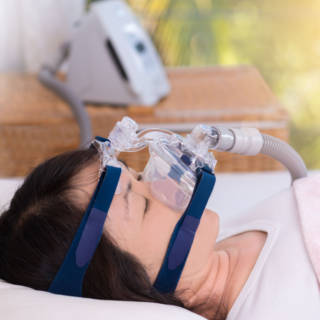
You have probably seen TV advertisements for CPAPs, a continuous positive airway pressure device. The machine provides air pressure greater than the surrounding air, so your air passages will stay open. There are many different types with a large selection of masks. So, if one doesn’t fit comfortably, keep trying until you find one that does. There are different variations in how much pressure and when it’s applied. Your doctor will help you find the one that works best for you.
Some people try using oral devices to help keep their airway open. Usually, they aren’t as effective as CPAP and work best for mild cases. Typically, you get these devices from your dentist and need to follow up frequently to ensure the device is still fitting correctly to guarantee you’re getting the maximum benefit.
If the devices don’t work or your apnea is severe, your doctor may recommend surgery. There are several types, like tissue removal, tissue shrinkage, jaw repositioning, implants, nerve stimulation or creating a new air passageway, or tracheostomy. Some of these procedures are still researched as treatment options.
Prevention
Self-care and prevention of sleep apnea are basically the same. If you’re overweight, the best thing you can do is lose weight and maintain a healthy one. Even if you’re not overweight, it’s still important to exercise for about 30 minutes most days of the week. Not smoking is essential because it significantly impacts your airway passages.
Don’t sleep on your back because your tongue and soft palate are more likely to block your airway by resting on the back of your throat. Instead, sleep on your side or stomach. Avoid drinking alcohol or using medications that have sedative qualities, like tranquilizers, because they can relax the muscles in the back of your throat. This is especially important if you have any risk factors for sleep apnea.
Sleep apnea is more than just snoring. It needs to be addressed to prevent more serious medical complications. If you have any questions or concerns about sleep apnea, please speak with your doctor. If you would like more information, please visit the National Institute of Health’s National Heart, Lung and Blood Institute’s sleep apnea page at https://www.nhlbi.nih.gov/health-topics/sleep-apnea