What can and can’t they do?
One topic that is always controversial is stem cells. Some people are for using them and others are against it. However, many people don’t fully understand what they’re all about. This is vital to know. So, what are stem cells? What can they be used for? What are the downsides?
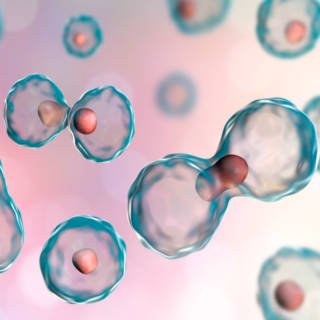 All of us start as only one cell, called a zygote (the term for a fertilized egg). The zygote divides into two cells, then four cells, and so on. At certain points in the developmental process, the cells begin to take on specific functions of different parts of the body. This process is called differentiation. Stem cells are cells that haven’t differentiated yet and can make an indefinite number of copies of themselves. When it divides, it can either remain a new stem cell (self-renewal) or turn into a differentiated cell. No other cell in the body has the natural ability to generate new cell types. Differentiated cells can only replicate into a similar cell type and have a limited number of times they can replicate before they begin to break down. There are several different types of stem cells, such as embryonic, perinatal, adult, and induced pluripotent. Researchers categorize them according to their potential to differentiate into other types of cells. Totipotent are those that can differentiate into all possible cell types. The first few cells that appear as the zygote fall under this classification. Pluripotent can turn into almost any cell. Multipotent means the cells can differentiate into a closely related family of cells. Oligopotent indicates the cells can differentiate into a few different cell types. Unipotent cells only produce cells of one kind (their own type); they’re still stem cells because they can renew themselves.
All of us start as only one cell, called a zygote (the term for a fertilized egg). The zygote divides into two cells, then four cells, and so on. At certain points in the developmental process, the cells begin to take on specific functions of different parts of the body. This process is called differentiation. Stem cells are cells that haven’t differentiated yet and can make an indefinite number of copies of themselves. When it divides, it can either remain a new stem cell (self-renewal) or turn into a differentiated cell. No other cell in the body has the natural ability to generate new cell types. Differentiated cells can only replicate into a similar cell type and have a limited number of times they can replicate before they begin to break down. There are several different types of stem cells, such as embryonic, perinatal, adult, and induced pluripotent. Researchers categorize them according to their potential to differentiate into other types of cells. Totipotent are those that can differentiate into all possible cell types. The first few cells that appear as the zygote fall under this classification. Pluripotent can turn into almost any cell. Multipotent means the cells can differentiate into a closely related family of cells. Oligopotent indicates the cells can differentiate into a few different cell types. Unipotent cells only produce cells of one kind (their own type); they’re still stem cells because they can renew themselves.
Embryonic stem cells come from embryos that are three to five days old. After this point, the cells begin to differentiate. During this period, an embryo is known as a blastocyst and has about 150 cells. The blastocyst consists of two parts: an outer cell mass that will become part of the placenta and an inner cell mass that will turn into the human body. The inner cell mass is where embryonic stem cells are found. Embryonic stem cells can differentiate into almost any cell type, making them pluripotent. They aren’t totipotent because they cannot become part of the extra-embryonic membranes or the placenta. It’s key to note that embryonic stem cells used for research don’t come from eggs fertilized in a woman’s body. Instead, they come from in vitro fertilization clinics. The doctors at these clinics fertilize several eggs in a test tube, to ensure that at least one survives. They will then implant a limited number of eggs to start a pregnancy. Rather than throwing away the left-over cells, some individuals choose to donate them for research purposes. These cells live and grow in special solutions in test tubes or petri dishes in laboratories.
Perinatal stem cells are found in the amniotic fluid and umbilical cord blood. These stem cells also have the ability to change into specialized cells. Amniotic fluid surrounds and protects a developing fetus in the uterus. More study is needed to understand the potential of these cells. Cord blood stem cells are collected from the umbilical cord after childbirth. They can be frozen in cell banks for use in the future and have been successfully used to treat children with blood cancers and certain genetic blood disorders.
Adult stem cells are also called tissue-specific or somatic stem cells (refers to non-reproductive cells in the body). They have a misleading name because they’re also found in infants and children. The cells are more specialized than embryonic stem cells but remain in a non-specific state until the body needs them for a specific purpose. They can be difficult to find because they can stay non-dividing and non-specific for years. However, since the body is constantly renewing its tissues, adult stem cells regularly divide to produce new tissues for maintenance and repair. A good example of this is when you cut your arm and it heals. Similarly, to embryonic stem cells, adult stem cells can self-renew indefinitely. These types of stem cells have been found in most tissues throughout the body, including the brain, bone marrow, blood/blood vessels, skeletal muscles, skin, and the liver. Scientists have known about adult stem cells for years and have classified them into numerous types; some examples are mesenchymal, hematopoietic, neural, epithelial, and skin. Mesenchymal stem cells (MSCs) come from the connective tissue or stroma surrounding the body’s organs and other tissues. These have been used to create new body tissues, like bone, cartilage, and fat cells. Hematopoietic stem cells, which are found in bone marrow and make new red blood cells, white blood cells, and other types of blood cells. They first were extracted and used for blood production in 1948. In 1968, this procedure was expanded when the first adult bone marrow cells were used in clinical therapies to treat blood disease. Doctors now routinely use them to treat diseases, like certain cancers. Until recently, researchers thought adult stem cells could create only similar types of cells, but emerging evidence indicates that they may be able to create various types of cells. There are concerns about their versatility and durability when compared to embryonic stem cells. Adult stem cells are more likely to contain abnormalities due to environmental hazards, such as toxins, or from errors attained during cell replication.
Adult stem cells that have been altered to have properties of embryonic stem cells are called induced pluripotent stem cells (iPSC). This means that scientists can reprogram adult stem cells so they act similarly to embryonic stem cells. This is a significant breakthrough for many reasons. The first is that it could allow researchers to use reprogrammed cells instead of embryonic stem cells. The next most important issue is that scientists are hoping to take stem cells from someone and use them to treat a disease they have. By using their own cells, it’ll decrease the chances of the body’s immune system from rejecting the new cells. However, since the technology was discovered in 2006, not much is known about how altered adult cells will affect humans.
Stem cells are grown in a lab. To accomplish this, scientists first extract samples from adult tissue or an embryo before placing these cells in a controlled culture where they will divide and reproduce but not specialize further. This is called a stem-cell line. The process of cells in a stem cell line growing but not differentiating into specialized cells is key. Ideally, they remain free of genetic defects while continuing to create more stem cells. Clusters of cells can be taken from a stem cell line and frozen for storage or shared with other researchers. Researchers have discovered ways to direct stem cells to become specific types of cells; this is called directed differentiation. However, they’re still trying to figure out how to ensure that the stem cells will differentiate into the specific cell types desired because embryonic stem cells can grow irregularly or specialize in different cell types spontaneously. So, if not properly directed, these stem cells may overgrow and cause tumors when injected into a patient. Obviously, controlling the outcome is vital to being able to use stem cells as therapeutic treatment. Once this is mastered, specialized cells can then be implanted into a person and could repair defective tissue or organs. This type of treatment is known as stem cell therapy, or regenerative medicine, because it promotes the repair response of diseased, dysfunctional, or injured tissue using stem cells or their derivatives.
Besides replacing damaged organs or tissues, scientists are looking at several other uses for stem cells, such as replacing organs that don’t work properly, researching causes of genetic defects in cells, exploring how diseases occur or why certain cells develop into cancer cells, and testing new drugs for safety and effectiveness. An area that could be revolutionized with stem cells is organ donation. Many people rely on having a donated organ or tissue to replace damaged ones. Unfortunately, more people need these than what people are willing or able to give up. Stem cell therapy could potentially lead to a sustainable method of replacing organs and tissue. Scientists have discovered that switching a particular gene on or off can cause it to differentiate. By understanding this, it’s helping them to investigate which genes and mutations cause which effects, knowing this could lead to a cure for many diseases, like type 1 diabetes, traumatic spinal cord injury, stroke, severe burns, rheumatoid arthritis, heart disease, hearing loss, retinal disease, Huntington’s disease, and Parkinson’s disease. With the help of stem cells, scientists believe that they could find the cause of cancer initiation and progression, which means they could potentially get rid of the disease. Another use for stem cells is testing the safety and efficacy of new, investigational drugs. This could be done before using the drugs in people and would eliminate the need to test them on animals. For this method to be accurate, the stem cells must be programmed to acquire properties of the type of cells targeted by the drug. By using iPCS, researchers could create patient-specific cell populations that would allow them to replicate disease conditions. The issue is that the conditions must be identical to actual patient situations to be able to compare results accurately. Currently, this is where the research is falling short. However, the future of this type of treatment is promising enough that the pharmaceutical industry is supporting further development.
Many obstacles must be overcome before the potential uses of stem cells in cell therapy will be accomplished. The first task is finding an appropriate source of stem cells. The process of identifying, isolating, and growing the right kind is presently laborious. The next issue is creating the right conditions so that the cells differentiate into the specialized cells required for a particular therapy. The final concern is developing a system that delivers the cells to the right part of the body and once there, they must be encouraged to integrate and function in concert with the body’s natural cells. Depending on the type of stem cell used, the body’s immune system may need to be suppressed to minimize the immune reaction set off by the transplanted cells.
The use of embryonic stem cells extracted from human embryos for research has raised several questions and issues about its ethics. The main topic is that during the harvesting process, the embryo is destroyed. Some people against embryonic stem cell research believe that an embryo is a living human being and don’t think fertilized eggs should be used for research. They argue that embryos have the same rights as every other human and these rights should be protected. Some supporters of embryonic stem cell research believe that the embryos are not yet humans. They argue that the fertilized eggs created during in-vitro fertilization would be discarded anyway, so they could be put to better use for scientific research. These individuals also point out that researchers receive consent to donate the embryos from the couple whose eggs and sperm were used to create it. Adult stem cells don’t present any ethical problems, especially with the breakthrough discovery of iPSCs. This means there may be less of a need for human embryos in research, which could ease concerns and opposition. iPSCs are also appealing because it avoids the issue of lifelong immunosuppression, which is needed if using donor stem cells. Right now, researchers still need access to embryonic stem cells because the study of iPCS cells is in its early stages and reprogramming may have serious limitations that aren’t known yet.
In the United States, no federal regulation has ever explicitly banned stem cell research, but regulations have placed restrictions on public funding and use. Certain states have placed bans on the creation or destruction of human embryos for medical research. In March 2009, President Barack Obama released Executive Order 13505, allowing the National Institutes of Health (NIH) to begin funding research that uses embryonic stem cells. After this, the NIH published guidelines to establish the policy under which it would fund research that is morally responsible and scientifically relevant. The guidelines define what an embryonic stem cell is and how it may be used in research. It provides recommendations for the donation of these cells and states embryonic stem cells from embryos created by in vitro fertilization can be used only when it is no longer needed by the couple who authorized its creation.
If you want, you can take advantage of stem cell benefits starting now. Anyone can donate stem cells to help a loved one or possibly for your own future use. Donations can come from several sources. One option is directly removing bone marrow from the hip or pelvic bone through a biopsy. After being retrieved, the stem cells are isolated and stored at a cell bank. An alternative option is to obtain peripheral stem cells. This involves receiving several injections that cause bone marrow to release stem cells into the blood. Next, blood is removed from the body, where a machine filters out the stem cells before returning the blood to the body. After being separated, the stem cells are stored until they’re needed. It’s a good idea for expecting parents to consider harvesting stem cells from umbilical cord blood after your baby is delivered. There’s no harm to the baby and it could be helpful in the future. A key consideration with any of these is that the collecting of stem cells is expensive.
Many stem cell therapies are being touted. The concern is that not all of them are safe. Just because a therapy is experimental doesn’t automatically mean that it’s part of a research study or clinical trial. It’s also essential to realize that unproven stem cell treatments can cause complications in the short- and long-term and may make your condition or symptoms worse. In addition, if you participate in an unproven or experimental treatment, it may make you ineligible for future clinical trials or treatment options. An additional consideration is the out-of-pocket expenses could be enormous since most insurance companies and government health programs don’t cover the cost of experimental treatments. If you’re contemplating a stem cell treatment, check with the provider or the Food and Drug Administration (FDA) that the product has approval, which means that it was made in a way that meets with FDA standards for safety and effectiveness.
While stem cell therapies are currently limited, they have enormous potential. Given their unique regenerative abilities, treating a diverse range of diseases with stem cells in the future is a real possibility. However, much more work needs to be done to better understand how to use them. Someday, instead of treating symptoms of diseases, we’ll be able to treat the cause of conditions thanks to stem cells.